 
The patient underwent a C2 to T4 laminectomy and posterior spinal fusion. Images are shown below ( Figures 1 and 2).Ĭervical myelopathy from ossification of posterior longitudinal ligament (OPLL). MRI of her cervical/thoracic spine revealed significant ossification of the posterior longitudinal complex enlargement resulting in severe central canal stenosis and multilevel cord compression from C2-3 to T2-3. Magnetic resonance imaging (MRI) of the brain, cervical and thoracic spine, with and without contrast, was performed.Ī previous MRI, which was done at an outside facility, of her lumbar spine revealed moderate canal stenosis at L2-S1 with some ossification of the Initial workup including thyroid-stimulating hormone (TSH) blood test, vitamin B12 level, methylmalonic acid, homocysteine, serum copper, and human T-lymphotropic virus 1 (HTLV-1) antibody were all normal. She was diffusely hyper-reflexic with sustained right ankle clonus, positive crossed adductor, suprapatellar, and pectoralis reflexes, bilateral plantar extensor responses, and positive Hoffmann’s signs. 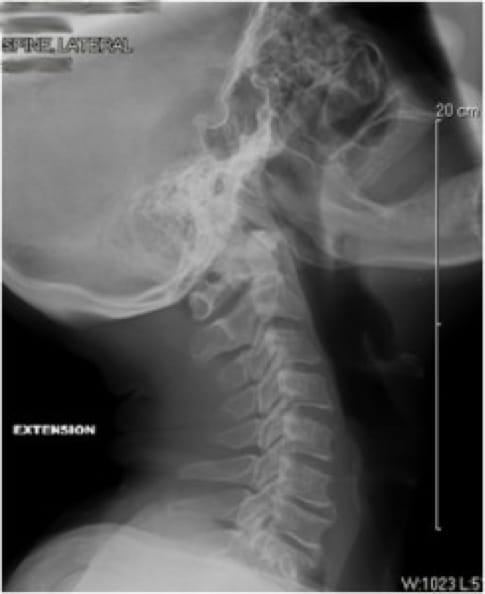
She exhibited a spastic gait on the right with inability to heel walk or tandem walk. There was slight decrease in joint position and vibration sensation at the toes bilaterally. Pertinent findings on examination revealed increased muscle tone, predominantly in the right lower extremity, mild right hip flexion, knee flexion, and ankle dorsiflexion weakness. As a physician, she became extremely concerned and anxious that she might be developing a serious, progressive, degenerative neurological ailment such as multiple sclerosis or amyotrophic lateral sclerosis. She denied back or neck pain, radicular pain, bowel or bladder symptoms, cranial nerve related complaints, or other neurologic deficit. Over the next few weeks, she noted worsening in her gait, the inability to run or walk long distances, and the occurrence of cramping pain in her legs. The patient had recently vacationed in Africa, when she noted the occurrence of pain in her right thigh, followed by a noticeable limp in her gait. Each of these cases reveals an unexpected diagnosis and highlights the importance of a broad differential diagnosis when confronted with a patient who may exhibit signs of myelopathy.Ī 44-year-old female physician with a history of hyperthyroidism was referred to our neuromuscular division for evaluation of abnormal gait, right leg weakness and cramping of five weeks’ duration. All patients were seen at the Neuromuscular Division of the Department of Neurology at the University of Southern California Keck Medical Center, US. Here, we present and discuss three unusual cases presenting with myelopathy, within a three-month period, and their respective workup and uncommon diagnoses. This will ensure appropriate and timely management and counseling. 
It is critical that clinicians use their clinical knowledge and utilize appropriate diagnostic studies in order to arrive at the correct diagnosis. Differential diagnosis classically includes structural etiology, demyelinating, metabolic, nutritional, inherited, and degenerative causes, resulting in a vast array of pathophysiologic processes, underlying myelopathy ( Table 1). Myelopathy is a common diagnosis often made by clinical neurologists and can be a cause of significant disability. Myelopathy, ossification of the posterior longitudinal ligament, adrenomyeloneuropathy, copper deficiency myelopathy, gait disturbance Article: These three diagnoses differ in etiology and highlight the need for a close and thorough examination and workup to arrive at the correct diagnosis, which in turn leads to appropriate treatment.Ĭompliance with Ethics: Informed consent was obtained from all patients for being included in the case study. All three cases initially presented with gait disturbance, and the ensuing workup revealed rare diagnoses in two out of the three cases. In this paper, we present three cases of myelopathy due to three different etiologies and pathogeneses. Depending on the etiology underlying the myelopathy, treatment may be surgical, medical, or supportive. Myelopathy is a common neurologic finding and presentations may vary widely. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
